Vikings Disease or Dupuytren’s \du-pwe-tran\ contracture is a fairly common disorder of the fingers. It most often affects the ring or little finger, sometimes both, and often in both hands. The disorder may occur suddenly but more commonly progresses slowly over a period of years and usually doesn’t cause symptoms until after the age of 40.
Anatomy of the hand
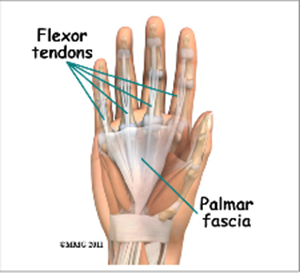
The palm side of the hand contains many nerves, tendons, muscles, ligaments, and bones. This combination allows us to move the hand in many ways. The bones give our hand structure and form joints. Bones are attached to bones by ligaments. Muscles allow us to bend and straighten our joints. Muscles are attached to bones by tendons. Nerves stimulate the muscles to bend and straighten. Blood vessels carry needed oxygen, nutrients, and fuel to the muscles to allow them to work normally and heal when injured.
Dupuytren’s Contracture explained simply
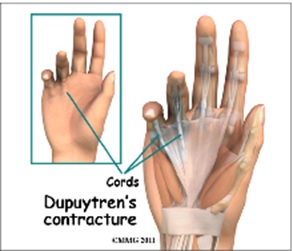
Dupuytren’s contracture is a thickening and shortening of tissue in the palm, resulting in the affected being unable to straighten some or all fingers (typically the ring finger is first affected, followed by the little finger and finally the middle finger). One of the first symptoms to look out for is a hard lump that appears on the palm, usually close to the base of the ring or little finger.
Thankfully, Dupuytren’s is not usually painful, however the main concern as it develops is that you cannot use the affected fingers properly. Everyday tasks with Dupuytren’s can be very difficult, especially in the later stages.
Causes
People who smoke have a greater risk of having Dupuytren’s contracture. Heavy smokers who abuse alcohol are even more at risk.
Recently, scientists have found a connection with the disease among people who have diabetes. It has not been determined whether or not work tasks can put a person at risk or speed the progression of the disease.
Symptoms of Vikings disease
- It is commonly both hands (45%) but can affect one hand.
- It starts with pitting and thickening of the palmar skin and underlying subcutaneous tissue, with loss of mobility of the overlying skin.
- Next a nodule forms which are firm and painless and fixed to the skin and deeper fascia. The nodule is palpable and later becomes visible.
- A cord (a linear thickening that can resemble a tendon) then develops which begins to contract over months to years.
- The contraction of the cord pulls on the metacarpophalangeal (MCP) and proximal interphalangeal (PIP) joints and leads to a progressive flexion deformity in the fingers.
- The deformity can affect activities of daily living and occupation. The stage at which the patient presents will depend upon the tolerance of this and is likely to depend upon the degree to which work or hobbies may be affected.
Diagnosis
At the Centre for Musculoskeletal Medicine we will ask you:
- The history of your problem, such as how long you have had it, whether you’ve noticed it getting worse, and whether it has kept you from doing your daily activities.
- Examination of your hands and fingers by looking at and feeling the palm of your hand and your fingers. Abnormal fascia will feel thick. Cords and small nodules in the fascia may be felt as small knots or thick bands under the skin. These nodules usually form first in the palm of the hand. As the disorder progresses, nodules form along with the finger.
The progression of the disorder is unpredictable. Some patients have no problems for years, and then suddenly nodules will begin to grow and their finger will begin to contract.
Treatment for Vikings disease
What can be done for the condition?
To help with pliability and release, healing of the palmer fascia:
- Ultrasound and soft tissue
- Dry needling
- Special stretches of the palmar fascia
- Shock wave therapy of the palmer fascia
- Articulation of the hand to mobilise stiff joints


